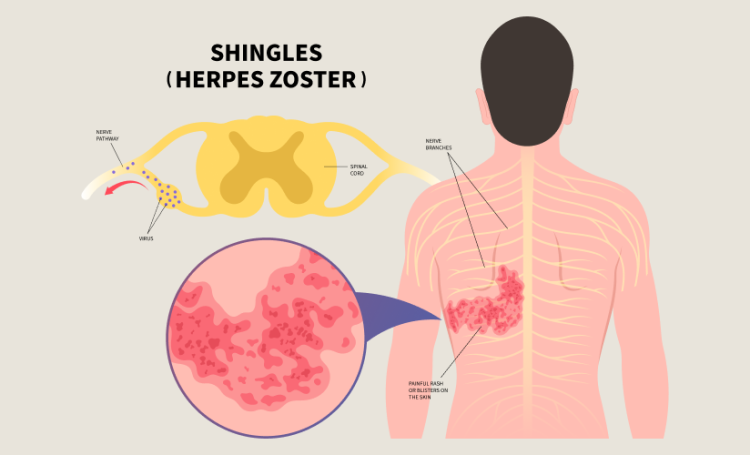
Zoster paralysis is one of those conditions most people never hear about until it happens. When people think about shingles, they usually picture a painful rash. However, zoster paralysis shows that the virus can go much deeper, affecting how your muscles actually work.
In simple terms, zoster paralysis happens when the same virus that causes shingles interferes with the nerves that control movement. While it is rare, it can be frightening because it leads to sudden weakness in parts of the body.
What is zoster paralysis and why it happens
Zoster paralysis develops when the varicella-zoster virus reactivates and spreads beyond the sensory nerves into motor nerves. These motor nerves are responsible for muscle movement, so when they are affected, weakness follows.
Most people first notice shingles through pain or a burning feeling, followed by a rash. However, in cases of zoster paralysis, muscle weakness can appear around the same time or shortly after. In some situations, the weakness may even show up before the rash, which can confuse both patients and doctors.
The virus itself stays hidden in nerve cells after a person has had chickenpox. Later in life, especially when the immune system weakens, it can reactivate and cause complications like this.
Zoster paralysis symptoms to watch for
The signs of zoster paralysis are usually quite noticeable once they begin. Most people experience weakness in a specific part of the body, often where the shingles rash appears.
Some of the common symptoms include:
- Sudden weakness in an arm or leg
- Reduced sensation or unusual sensitivity
- Pain that comes before or with weakness
- Changes in reflexes
In many reported cases, the arms are affected more often than the legs. This can make everyday tasks like holding objects or lifting items difficult.
Why zoster paralysis can be missed
One of the biggest challenges with zoster paralysis is that it does not always look like a shingles complication at first. Doctors may initially think of conditions like stroke, nerve injury, or spinal problems.
Things become even more confusing when the rash appears late or is not very visible. There are also rare cases where shingles occurs without any rash at all, making diagnosis even harder.
Because of this, some patients may not get the right treatment immediately.
How doctors diagnose zoster paralysis
Diagnosing zoster paralysis usually involves looking at both symptoms and medical history. Doctors will ask about recent pain, rashes, or previous shingles infections.
They also rely on special tests like nerve conduction studies and electromyography. These tests help show how well the nerves and muscles are working and can confirm if there is nerve damage.
Research shows that most patients with this condition have clear changes in both motor and sensory nerve function.
Imaging tests such as MRI can also help by showing inflammation around the affected nerves.
Treatment and recovery for zoster paralysis
The good news is that early treatment can make a big difference. Doctors often combine several approaches to manage the condition and support recovery.
Treatment may include:
- Antiviral medication to control the infection
- Pain relief to manage discomfort
- Anti-inflammatory drugs like steroids
- Physical therapy to rebuild strength
Recovery can take time, often several months. However, many patients regain strength with proper treatment and care.
Who faces a higher risk
It is more likely to affect certain groups of people. These include older adults and individuals with weakened immune systems.
People undergoing treatments like chemotherapy or those with chronic illnesses also face a higher risk. That said, anyone who develops shingles could potentially experience this complication, even though it remains uncommon.
Why understanding zoster paralysis matters
Although zoster paralysis is rare, its impact can be serious. Losing strength in a limb can affect daily life, independence, and overall well-being.
Awareness is key. When people recognize the signs early and seek medical help quickly, the chances of recovery improve significantly.
It is a reminder that shingles is not always just a skin condition. It can affect the nerves that control movement and lead to sudden muscle weakness.
The condition may be uncommon, but understanding it can help people act quickly if symptoms appear. With early diagnosis and the right treatment, recovery is possible, and long-term effects can be reduced.